Peyronie’s disease is a disorder involving scar tissue formation under the skin of the penis, causing penile curvature and erectile dysfunction. What are its causes and how is it being treated? Here’s everything you need to know.
It was Dr. de la Peyronie, a first-surgeon to King Louis the 15th, who 250 years ago described the disorder which now bears his name, and the methods of its treatment. Peyronie’s Disease (PD) is an acquired disorder (unlike the congenital one which develops in utero), characterized by curvature in the penile shaft which might lead to sexual dysfunction. It develops when firm scar tissue called plaque builds up in different places along the tunica albuginea (the membrane enveloping the erectile tissues) and replaces the elastic tissue that allows the penis to becomes enlarged, hardened, and erect during an erection. As it develops, the scar tissue pulls on the surrounding tissues and causes the penis to curve during an erection.
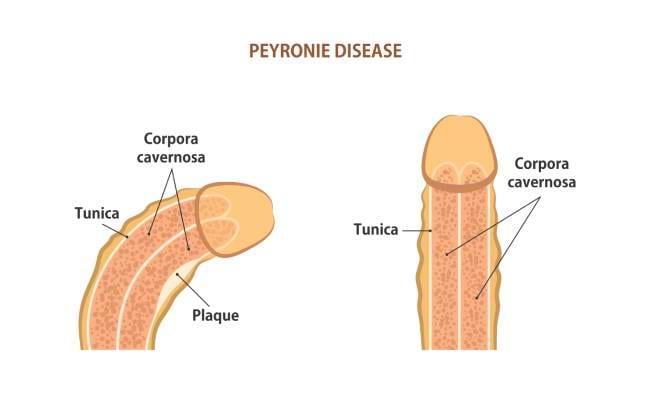 Fig 1: Penile curvature during erection due to scar tissue formation (plaque).
Fig 1: Penile curvature during erection due to scar tissue formation (plaque).
PD occurs in 3-9% of the men, usually from the age of 40. Although its prevalence increases with age it can also occur in teenager boys, and its severity varies from person to person.
Symptoms of Peyronie’s Disease
The most common symptom of Peyronie’s disease is the development of palpable scar tissue (plaques) in the tunica albuginea. Later on, the plaques undergo a process of calcification and become very hard. Usually, scar tissue forms on the top of the penis causing it to bend upwards when erect, but it may also form on the bottom or sides and cause the penis to curve down or to the left or right. In certain cases, the plaques form all around the shaft of the penis causing it to narrow in an hourglass-like shape – a deformity referred to as “bottle-necking”.
Additional symptoms, which might give rise to erectile and sexual dysfunction, include: softer erections, painful erections and painful intercourse, a shorter penis during the erect state and occasionally during the flaccid state as well.
In a research study published in the journal Urology, it was noted that more than 54% of the men diagnosed with PD also report experiencing ED, although not all cases PD necessarily involve problems with sexual intercourse.
PD has psychological effects as well and research show that numerous men affected by the disease cope with some level of stress and concerns about their ability to engage in satisfying sexual activity and about their physical appearance. Many men experience anxiety prior to or during sexual intercourse, loss of confidence and sometimes even depression and reduced quality of life.
The Acute Phase and the Chronic Phase
PD occurs in two stages, often referred to as ‘the acute phase and chronic phase’ of the disease. Each phase is characterized by different symptoms:
- Acute phase – also referred to as the early or inflammatory phase. During this phase, plaques develop on the membrane of the penis as part of an acute inflammatory process. The man usually feels discomfort or pain even when the penis is flaccid, and the organ begins to curve or bend. When scar tissue begins to form erection might become painful. This phase can last usually up to 18 months, but for most patients the pain will subside within 5-7 months.
- Chronic phase – this is the phase following plaques’ formation which usually begins 12 – 18 months following the occurrence of the first symptoms of PD. During this phase, the plaques are no longer actively growing and the curvature stabilizes. The pain and discomfort normally subside, though some men continue to experience ED, occasionally more severely.
It’s important to note that according to studies, in 10-15% of the cases the condition will resolve spontaneously a year after diagnosis, in 40% of the cases it will remain unchanged while 45% of the cases will result in disease aggravation.
Why Does It Happen? The Causes of Peyronie’s Disease
The cause of Peyronie’s disease is largely unknown, but according to the accepted presumption PD develops following trauma, such as (though not necessarily) bending the penis during penetration or vigorous masturbation. Trauma during other circumstances include sport injuries or an accident. As a result, micro-injuries in the tunica albuginea cause localized bleeding within its layers, leading to an inflammatory response which eventually results in scar tissue formation. Some patients are not even aware of such micro-injury at the time it occurs, and many cannot remember a specific incident just before symptoms began.
Apart from that, some researchers claim that its possible that PD has an autoimmune background, that is, the immune system attacks cells in the tunica albuginea causing an inflammatory response and scar tissue formation.
According to medical literature, several risk factors are associated with an increased risk of developing PD, including:
- Connective tissue diseases – such as Dupuytren’s contracture – a condition which occurs in a third of PD’s patients, where connective tissue in the palms shortens and thickens; Scleroderma – a condition that causes swelling or pain in muscles and joints due to abnormal growth of hard patches of connective tissue; Plantar fasciitis – inflammation of the ligament that connects to the heel’s bone in the foot.
- Prostate cancer surgery – some medical exert believe that PD is in fact related to ED development following surgery for prostate cancer
- Diabetes related ED – increases the risk of PD development by 4 – 5 times compared to the general population
- Older age
- Family history of PD – in families were first-degree relatives (a father or brother) have PD the chances of developing the disease increase significantly
Current Treatments for Peyronie’s Disease
The various treatment options will depend on the disease’s phase: during the acute phase treatment will focus on an attempt to slow down disease progression and reducing pain. During the chronic phase treatment will focus on straitening the penis, and when necessary, restoring the ability to have sexual intercourse.
In cases in which the plaques are small, there is mild or no penile curvature and no pain nor problems with sexual intercourse and urination – it is possible that treatment will not be required.
If treatment is needed, a urologist will decide on surgery or otherwise nonsurgical treatments, depending on the severity of symptoms and the phase of the disease.
1. Non-surgical treatments are suitable for the acute phase. They are based on medications (acting in various anti-inflammatory mechanisms) or penile injections directly into the plaques.
- Injections may be based on:
-
- Collagenase – an enzyme that helps break down collagen in the plaques, thus reducing penile curving and improving erectile function. If successful, this treatment might replace surgery.
- Antihypertension medication – may reduce pain and penile curving when injected into the plaque.
- Interferon-alpha 2b– interferon is a protein made by immune cells. Studies have shown that it can reduce pain, penile curvature and plaque size.
- Oral medications – Currently there are no oral medications that treat penile curvature effectively. There is drug treatment (used for treating Dupuytren’s contracture) which may reduce the size of the plaques. Non-steroidal anti-inflammatory medications may be given for reducing pain.
Apart collagenase, which is unavailable in Europe, all other types of injections and medications have not been proved as significantly helpful.
Nondrug medical therapies that that are still being studied include:
-
- mechanical traction and vacuum devices—based on stretching or bending the penis to reduce curvature
- shockwave therapy—directed at breaking the plaque and pain reduction
2. A minority of the patients who suffer from a significant penile deformity or substantial erectile dysfunction will require surgical treatment to straighten the penis, preserve its length and erectile function. The success rates of surgical treatments are considered very high:
- If there is no erectile dysfunction – surgery will focus on straightening the penis by shortening the longer side. Another possibility is plaque removal and its replacement with a healthy tissue taken from another part the body or from a synthetic source, in order to restore part of the original length of the penis.
- In case of erectile dysfunction – penile implants may be considered. There are cases in which penile implant alone straightens the penis. If not, it may be combined with one of the two aforementioned surgeries.
The Company hereby clarifies that the information contained on the website is for informational purposes only, and is not intended to be a substitute for professional medical and healthcare advice, and does not constitute medical advice or opinion. Always seek the advice of your physician or other qualified health provider with any medical condition or question you may have regarding a medical condition.